Learn About The RESTORE Advanced Infusion Difference...
Restore | Reboot | Recover...with RESTORE


How We Developed RESTORE and Why RESTORE is better than ketamine
The question of why RESTORE is better than ketamine seems like a simple one, but many factors need to be considered before making such an assessment. We will explore how and why the new RESTORE program offers significant advantages over typical methods for administering ketamine infusions in patients who suffer from mood disorders such as depression, anxiety, bipolar disorder, or PTSD.
It seems like a simple question, but it must be put into a broader context to fully appreciate the unique advantages of the new RESTORE infusion program over regular ketamine infusions. There are at least five major factors that can limit the effectiveness of a ketamine infusion. We need to review a little history regarding the origin of the ketamine infusion, how the ketamine is given, and who is administering it to understand better why RESTORE is a significant improvement over a regular ketamine infusion.
First, a little history about ketamine
It surprises many to learn that the standard ketamine infusion currently used around the country today was not developed to treat depression. It was developed as part of a research protocol at Yale University in the late 1990s to study the possible role of glutamate in the symptoms experienced by patients who had schizophrenia.
The Psychiatry Department at Yale was aware of earlier research studies in animal models that suggested glutamate may play a crucial role in this condition. It had been challenging to study because very few available drugs could safely alter glutamate release in humans. The one medication used clinically and known for doing so is ketamine - Parke-Davis developed this anesthetic agent in 1962. The FDA approved ketamine for use among children and adults in 1970. They were familiar with its safety profile within anesthesia practices over the preceding 25 years. They had gained insights from earlier studies in animal models and decided it would be the most appropriate medication for the study.
The Yale psychiatrists, unfamiliar with the use and administration of this medication, approached my department (Anesthesiology) to collaborate on the study by formulating an ultra-low dose infusion protocol for ketamine. The goal was to determine if it could produce symptoms like those seen in schizophrenia without adverse effects on subjects' health or physical condition. Should that prove successful, researchers would have a new way to investigate deeper into the causes of these severe mental disorders. And thereby lead to more effective treatments.
The Anesthesiology Department then determined the lowest blood level (serum concentration) of ketamine necessary to produce apparent symptoms that mimic those seen in schizophrenia. However, they found it technically complex and expensive to directly measure these blood concentrations for each person undergoing infusions. So, they developed a simplified protocol where 0.5 mg of ketamine given per kilogram of general body weight, slowly provided over 40 minutes, would achieve peak levels between 150-185 ng/ml in approximately 75% of subjects.
Although the study's initial results successfully achieved the desired blood level, they did not reproduce any negative symptoms associated with schizophrenia. Instead, subjects reported feeling good and experiencing mild euphoria or "mild intoxication." Although this was an unexpected outcome, the researchers continued to explore the possibility that ketamine may have other potential uses.
Despite being disappointed with the failure of ketamine to produce a model to study schizophrenia, they continued exploring other conditions. One question that came up in 1999 was whether the same kind of beneficial effects would occur when given to people suffering from other mood disorders such as depression?
Ketamine as a possible treatment for depression
In 1999-2000, nine patients with severe "treatment-resistant" depression were given a single ketamine infusion by the Yale researchers. Remarkably, not only did they experience the same mild euphoria and feeling a little intoxicated, but many of the patients also reported a rapid and dramatic improvement of their depression in just a matter of hours following the infusion session. More surprisingly, the improvement continued for about a week after the infusion, far longer than the 2-4 hours that ketamine would typically remain in their system.
The scientists were perplexed about how ketamine, an anesthetic that blocks glutamate and NMDA receptors, could reverse depression but decided to publish their results. This study, published in the Journal of Biological Psychiatry in 2000, became a "landmark" study in the field of Psychiatry that changed our understanding and approach to treating mood disorders.
The medical community's initial response to the publication of this early study was unimpressive. Few researchers or clinicians saw its future implications. It wasn't until about six years later, in 2006, when Dr. Carlos Zarate and his team at the National Institute of Mental Health published a more extensive study. Using the same infusion protocol, they demonstrated the same remarkable benefits from ketamine. It wasn't until this study was published that the medical community noted ketamine's unique effects.
Soon many other prestigious medical and scientific institutions around the world began to study it more closely. But there was a problem. Although patients responded very quickly, usually within the hour or two following an infusion, and experienced immediate relief from depression, it was only effective for about one week afterward. They understood that it would not be practical or cost-effective for people with depression to undergo infusions every week to maintain the benefit.
The answer came four years later, in 2010 when researchers decided to see if they could prolong the improvement seen with ketamine by using an old and well-known treatment method: electroshock therapy (ECT). ECT is known for its long-term benefits, but it requires multiple sessions of ECT over two weeks before patients notice a prolonged improvement in mood; would this same approach work for ketamine?
Fortunately, it did – at least to some degree. The research found that if ketamine were administered with the same schedule used for ECT every other day for two weeks, the improvement would last about 28 days before each person would need another infusion to maintain the gains.
Since then, the simple infusion protocol of 0.5mg ketamine per kilogram given intravenously over 40 minutes became the "de facto" standard ketamine infusion treatment for major depression used by major university medical centers, researchers, and practitioners worldwide.
While this simple approach can be very beneficial for those that have failed to improve with conventional antidepressant therapy, many believe that it falls short of providing more than a "bandaid" type of relief requiring monthly infusions to maintain the benefit.
Surprisingly, few physicians or researchers have attempted to determine if other underlying metabolic factors could dramatically improve your response to a ketamine infusion.
Could ketamine be made to work even better?
Although I was initially impressed with the early results, it was apparent that there were many other factors involved that could influence how well the infusion worked. After all, most of us have taken over-the-counter or prescription medications at one time or another, and we know that most medicines come in various strengths for different conditions.
Prozac, for example, is an older and very commonly prescribed antidepressant that is supplied in various strengths, including 10mg, 20mg, 40mg, 90mg capsules. Drug companies do this because each person will metabolize the drug differently, some more slowly and others very rapidly, leading to very different levels of Prozac in their bloodstream. Also, some conditions may be more challenging to treat and require more medication or higher blood levels to be effective.
In addition to primary metabolism, it is also essential to consider each person's unique genetic traits. Some individuals may have variations in receptor sites where the drug works or lack critical neurotrophins (small proteins that affect nerve cell growth and development) that play a role in responding to ketamine.
Another factor that needs to be considered is potential drug-drug interactions. Whenever we start a new medication, our practitioner or pharmacist will also warn us about taking other medicines simultaneously and how they might negatively interact with each other. The same types of interactions are also applicable to ketamine. Several commonly prescribed medications can significantly reduce ketamine's effectiveness. Lamictal, for example, is a mood-stabilizer that is often added to an antidepressant regimen, can dramatically reduce ketamine's ability to work effectively.
It may have been logical and easier to think that a "one-size fits all" approach would work for ketamine treatments in the early days. Still, I soon realized many other factors to consider beyond just bodyweight before determining the best infusion protocol. What was needed was a more individualized, comprehensive, and precise approach.
How we improved the ketamine infusion
The first step in my investigation was determining if various other doses or specific blood levels of ketamine would be more effective or last longer. Once that was determined, the next question I asked myself was the length of time necessary to maintain that concentration for maximal results. Finally, I needed to determine what genetic, metabolic, or medication issues could affect, either positively or negatively, how well someone would respond to the infusion process.
Over seven years, I was able to identify and determine what those optimal levels were. I found that each individual has different needs regarding their requirements and response during an infusion. The time necessary to maintain them and how body metabolism, genetics, and medications would affect the serum concentration of ketamine achieved during an infusion. When these factors were considered and accounted for, the results were a unique and more effective infusion program - RESTORE.
RESTORE is the advanced and improved version of ketamine
To maximize the full potential of ketamine, I used the results of my long clinical investigation to develop RESTORE. The RESTORE program utilizes an individualized and unique methodology that includes optimal blood levels of ketamine, improved administration technique, synergistic neuromodulators, and a metabolic optimization protocol to achieve the best results.
Before we consider beginning an infusion, our team spends a significant amount of time determining if that person is a good candidate for the RESTORE program and in optimal metabolic and hormonal state to obtain maximal improvement.
Steps in the RESTORE Program
1. Metabolic Optimization
We have found that certain patients may benefit from a more detailed laboratory evaluation and metabolic optimization before receiving RESTORE. Often, these critical tests have not been performed by their doctor but are very important for those suffering from depression or anxiety and post-traumatic stress disorder (PTSD). These findings can contribute to the development of the mood disorder and help us tailor treatment modifications specific to your needs maximizing your response to the RESTORE infusion.
In some challenging or very complex cases, we also find it beneficial to obtain a highly specialized genetic profile (Genomind) that looks at serotonin, dopamine, and norepinephrine receptors. This assay also provides additional critical information concerning MTHFR, BDNF, and COMT genotype variants, which gives us essential insight for improving an infusion treatment plan outcome.
2. Synergistic Agents and Neuromodulators
In addition to metabolic optimization before therapy, the RESTORE infusion is unique in other vital ways. RESTORE utilizes a combination of ketamine combined with magnesium additives to make it more effective than ketamine alone. Magnesium acts as a synergistic agent or cofactor, working at the same NMDA receptor site as ketamine. However, it can have unusual paradoxical effects. It must be given at the correct time and in the proper ratio to have a maximal positive impact in the presence of ketamine. When provided correctly, it can increase the NMDA receptor site responsiveness to ketamine by a factor of 200 to 300 percent.
More than that, we have also employed additional neuromodulators to significantly increase the effectiveness of ketamine. Specific well-known molecules can augment the binding affinity of ketamine for its receptor targets. At the same time, others can enhance the downstream effects of BDNF and mTOR activation, which promote neurogenesis and synaptic plasticity. The addition of these “ketamine-promoters” can unlock the full potential of ketamine’s therapeutic effect.
3. Improved Infusion Administration
As we have already discussed - the "one-size-fits-all" approach still used today is not as effective as it could be. We have addressed that issue by radically updating the simple weight-based 40-minute infusion protocol to a more sophisticated and effective 3-stage variable rate infusion. Utilizing this approach, RESTORE achieves optimal blood levels much faster and maintains them for a more extended period than a standard ketamine infusion. By optimizing serum concentrations in this way, the RESTORE infusion achieves higher effective serum concentrations of the parent molecule ketamine and higher concentrations of the critical metabolites of ketamine known as HNK (Hydroxynorketamine) and DHNK (Dehydronorketamine).
Increasing the HNK and DHNK in the bloodstream is very important to our protocol because it is the secondary metabolites of ketamine, HNK, and DHNK, which promote neuroplasticity and synaptic connectivity achieving long-term improvement. These metabolites increase BDNF (brain-derived neurotrophic factor) - a "miracle grow" type of crucial molecule - and sustain higher levels over a more extended period to produce more profound and durable effects.
4. RESTORE Supplements
We have also found that post-infusion supplementation with those same and additional cofactors, in a specific ratio, continues to promote and enhance the benefits of the infusion. Utilizing our advanced program combined with the RESTORE supplement enhances the improvement and increases how long it lasts 300-600% over ketamine alone.
There is one more vital factor to consider
So far, we have only touched on the pharmacological aspects of ketamine, but it is essential to remember that it also produces a profound and unique psychological experience. The therapeutic benefits from a RESTORE infusion do not solely lie in optimizing ketamine concentrations but also in allowing people to have personal perspective-changing moments that may greatly aid recovery.
A RESTORE infusion is a unique process where each person can achieve personal insight and understanding of the factors and events underlying deep-seated issues. The other critical factor that can directly aid in the experience is the "set and setting" in which the infusion occurs and who is administering it...
5. Who is administering the infusion, and in what setting?
Unlike any other program in the world — we only see one person at a time — so you have our full and undivided attention while you are with us.
Many physicians providing ketamine infusion therapy today have relatively little clinical or research experience with the intricate pharmacology of the medication. They lack detailed insight into its actual mechanism of action (i.e., pharmacokinetics and pharmacodynamics). While some ketamine providers are more knowledgeable about ketamine than others, most of those administering ketamine have never experienced a ketamine infusion themselves and do not fully understand the shift in perception during an infusion session.
We do. Not only have we performed thousands of infusions over the years, being right by each person's side during the entire session, but we have also personally experienced what it feels like to have an infusion. Many of our patients have told us that their experience during a RESTORE session was one of the most critical life-changing events in their lives.
As someone who knows firsthand what it is like, I can tell you that a crucial part of the RESTORE infusion program is being with people who have shared a similar experience - having them right there with you during each session.
So, we understand better than most what the experience is like, and that's why you are never left alone, with a friend, or with a nurse just "checking in on you from time to time" during the RESTORE experience.
Although the RESTORE infusion program is much more sophisticated than a conventional ketamine infusion, the results — at least in our opinion — are well worth it.
We are committed to what we do. We will use all our knowledge, experience, and expertise to help you. And while we cannot promise success in every case, we can promise and guarantee that we will make every possible effort and take every step necessary to ensure that you have the best likely chances of recovery with RESTORE.
That is why RESTORE is better than ketamine.
The RESTORE Infusion Program:
More effective than ketamine infusions
85% improve with RESTORE vs. 70% improve with ketamine
Faster Acting than ketamine
Only 3 RESTORE treatment sessions over three days vs. ketamine - 6 infusions over two weeks.
Longer Lasting than ketamine
Up to 1-3 years with RESTORE vs. Only one month with ketamine between maintenance infusions.
And it is Less Expensive and More Convenient than ketamine infusions.
____________________________________
RESTORE is the new "Gold Standard" in ketamine-based therapy
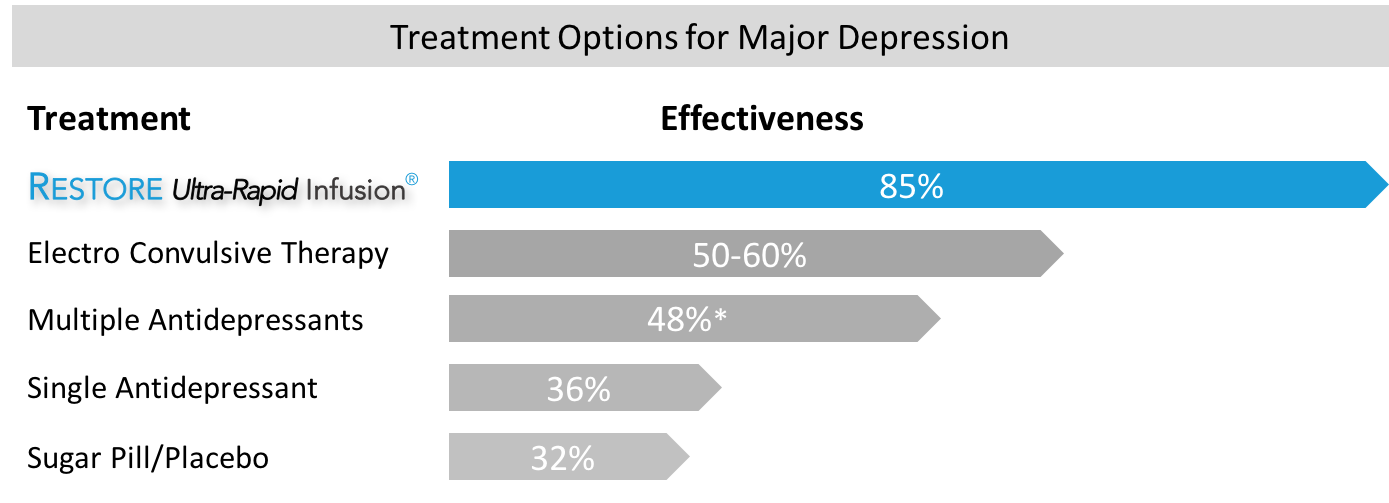
Depression
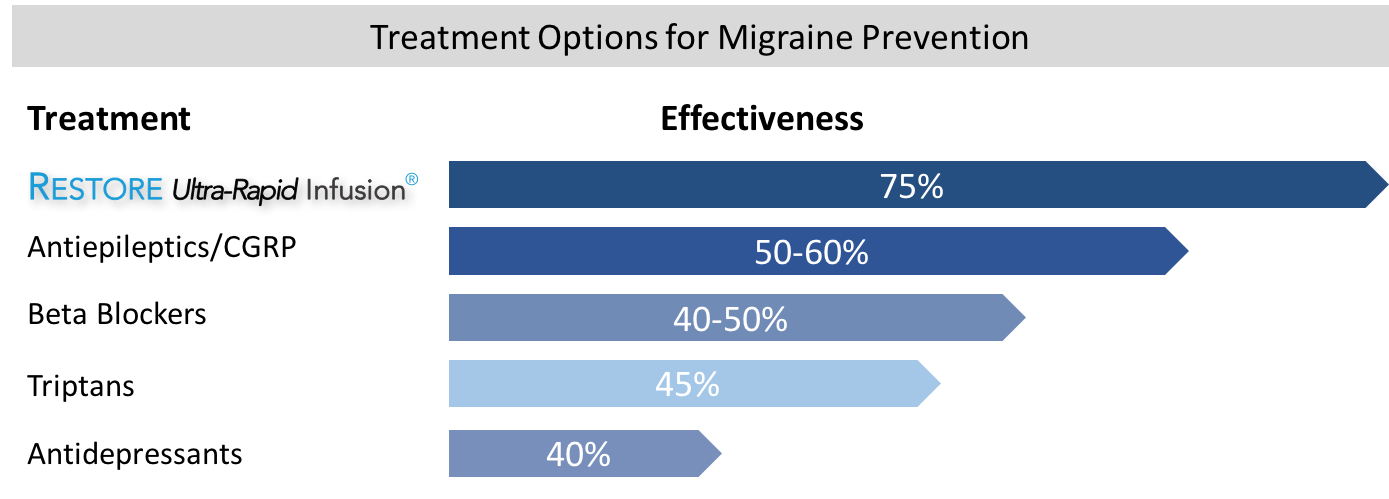
Migraine Headaches
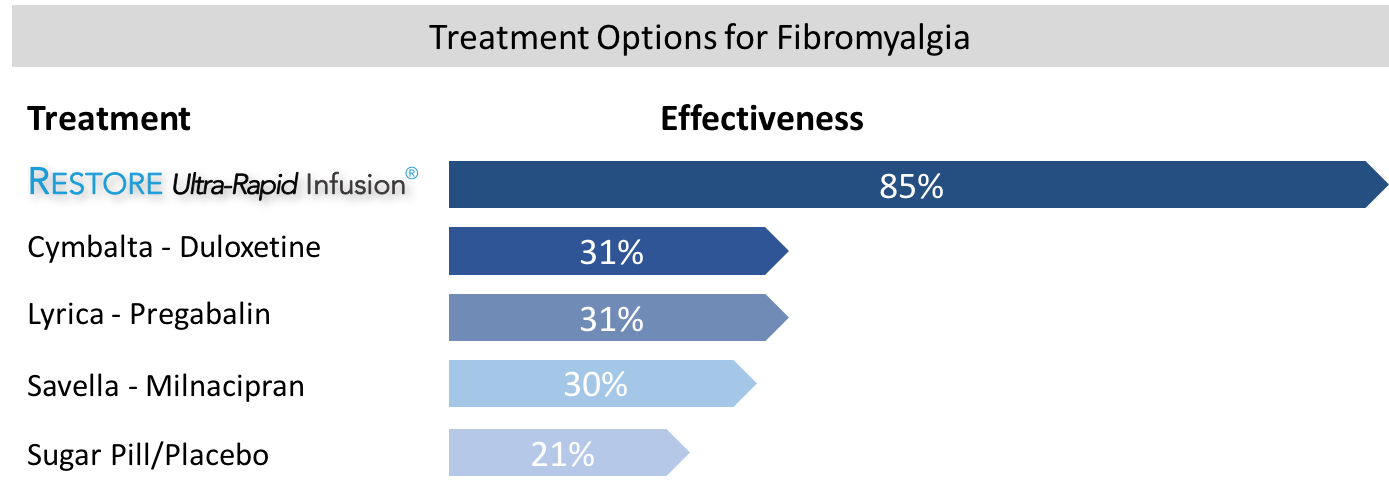
Fibromyalgia
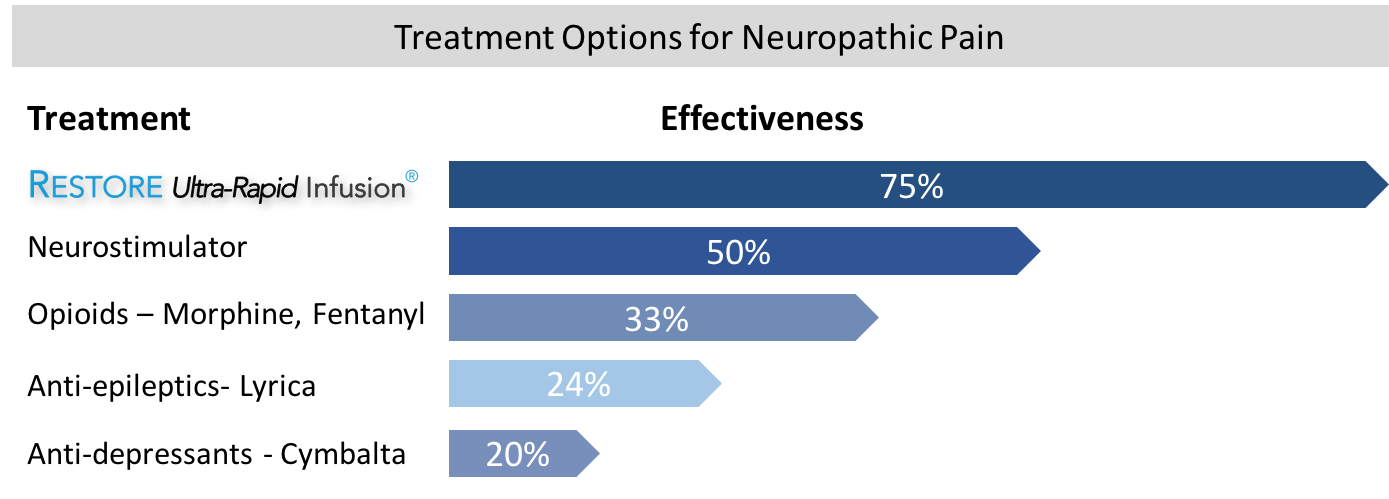
Neuropathic Pain - Including CRPS/RSD

 If you suffer from chronic pain or depression and have not had relief with prescription medication or other traditional treatment modalities, then the RESTORE Ultra-Rapid Infusion may be an option for you. We will be happy to provide you with an initial consultation to see if infusion therapy is right for you.
If you suffer from chronic pain or depression and have not had relief with prescription medication or other traditional treatment modalities, then the RESTORE Ultra-Rapid Infusion may be an option for you. We will be happy to provide you with an initial consultation to see if infusion therapy is right for you.
Just call us today:
800.850.6979
“The most important breakthrough in antidepressant treatment in decades”....
Thomas Insel, MD - Director, National Institute of Mental Health

